How to Foster Smarter, Person-Centered Care for High-Need, High-Cost Medicare Patients
While developing policy solutions to improve health outcomes for high-risk Medicare patients has challenged policymakers for years, we know that there are two primary factors that drive Medicare patients’ need for medical services: chronic conditions and functional or cognitive impairments. Medicare beneficiaries with these chronic conditions and functional or cognitive impairments often have the need for non-clinical supports, not covered under Medicare, which must be addressed to avoid expensive hospital stays and other potentially-avoidable care episodes. Medicare regulations and payment rules can often erect barriers to innovating evidence-based care designs to address those non-clinical needs, even for health plans and providers that accept financial risk for the cost of the beneficiary’s care.
There are two primary factors that drive Medicare patients’ need for medical services: chronic conditions and functional or cognitive impairments.
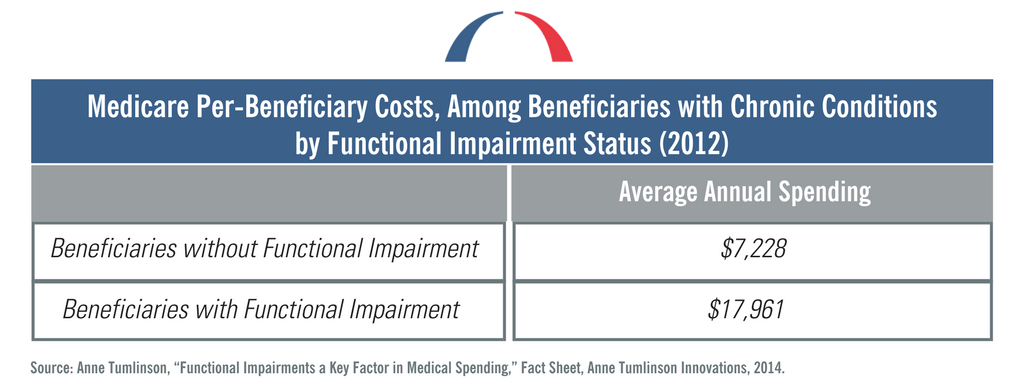
Prevalent chronic conditions include congestive heart failure, chronic obstructive pulmonary disease, and diabetes. Functional impairments are defined by difficulty in performing activities of daily living, such as transferring to and from bed without assistance. Cognitive impairments can include diminished intellectual capacity associated with dementia or Alzheimer’s, which can present safety concerns for the Medicare patient. Non-clinical supports that have the proven capability of preventing hospitalizations and utilization of other medical services include targeted care management, in-home meal delivery, home modifications, transportation to medical appointments, and long-term services and supports.
In a new preliminary report, the Bipartisan Policy Center examines these barriers and offers policy options aimed at improving the integration of Medicare-covered medical services with non-covered social supports in a variety of health care delivery models that provide care for high-need, high-cost Medicare beneficiaries who are not dually eligible for Medicaid. After consultation with experts and stakeholders concerning these policy options and related issues, BPC will finalize recommendations for Congress and the Centers for Medicare and Medicaid Services (CMS) in April 2017.

Allowing Targeting of Social Supports Coverage in Medicare Advantage: Among other options, Congress could make adjustments to the so-called “uniform benefit” rules that prohibit Medicare Advantage (MA) plans from targeting supplemental benefits, like non-emergent transportation or in-home meal delivery, to specific subpopulations of enrolled beneficiaries. Allowing this targeting of supplemental benefits could allow MA plans to better address the non-clinical support needs of their highest-risk enrollees in a financially viable manner within existing Medicare capitation payment amounts.
Using Quality Measures to Incentivize Integration of Non-Clinical Supports: CMS could establish quality metrics within the quality measurement sets for MA plans and Accountable Care Organizations (ACOs) that reward MA plans and ACOs that integrate non-Medicare-covered social supports into their care models for high-need Medicare patients.
Building a Better Risk Adjustment Model: CMS could also examine incorporating a functional/cognitive impairment factor into the Medicare risk adjustment model for MA plans and ACOs. Under such an approach, the risk scores (and corresponding risk adjustment payments) could be increased for Medicare beneficiaries who are certified as having functional or cognitive impairment, and decreased for those beneficiaries would do not have such impairments. This change could help address issues in the current Medicare risk adjustment model that result in significant underpayment for the highest-cost Medicare beneficiaries and substantial overpayment for the lowest-cost beneficiaries. As result of improved risk-adjusted payment adequacy for the highest-cost beneficiaries, MA plans and ACOs that care for high-cost Medicare patients could have the resources and incentives necessary to invest in the non-clinical supports that can help keep these patients out of the hospital and reduce lengthy subsequent nursing facility stays.
Offering Clarity on Program Integrity Rules and Restrictions: Finally, Congress could provide clarity to ACOs and patient-centered medical home providers to ensure that these provider organizations will not trigger violations of Medicare anti-fraud and program integrity rules when furnishing non-Medicare-covered supports at no charge for high-need Medicare patients.
As BPC continues to examine policy issues for high-cost patients and Medicare beneficiaries with chronic conditions, our team looks forward to continued collaboration with experts and stakeholders, so that we can develop policy solutions that ensure better health outcomes for patients and lower costs for the Medicare program.
Share
Read Next
Support Research Like This
With your support, BPC can continue to fund important research like this by combining the best ideas from both parties to promote health, security, and opportunity for all Americans.
Give NowRelated Articles
Join Our Mailing List
BPC drives principled and politically viable policy solutions through the power of rigorous analysis, painstaking negotiation, and aggressive advocacy.